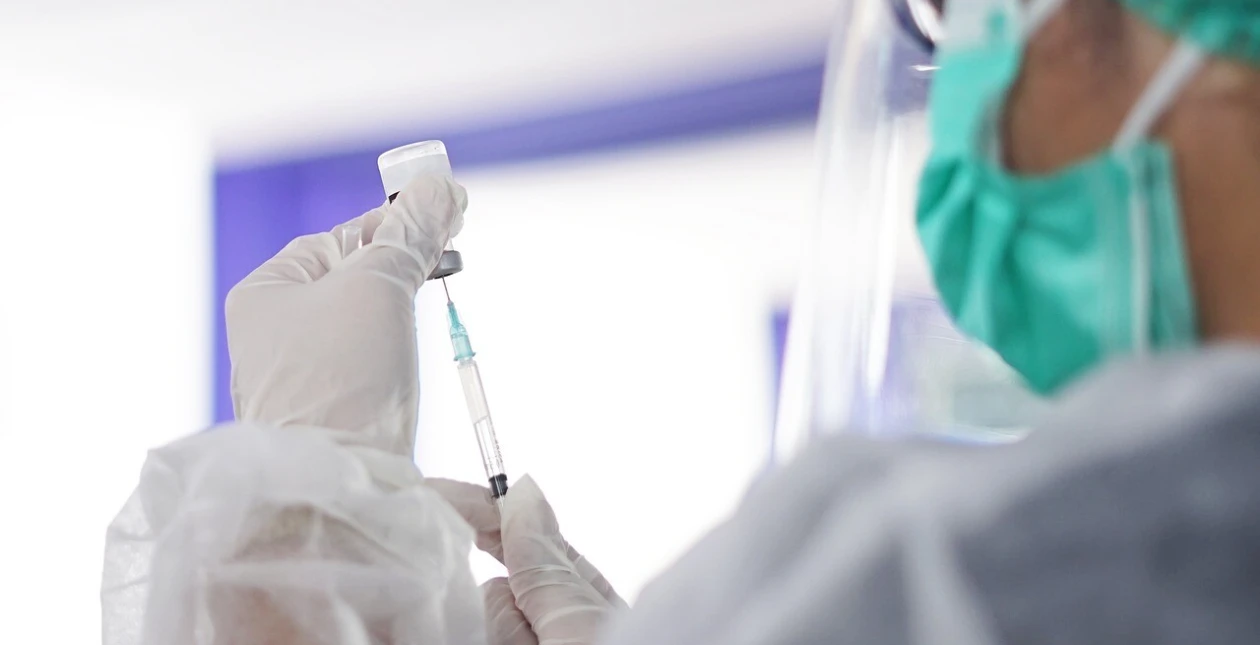
Motherhood is perhaps the most significant phase that women go through. The chance of having pregnancy-related issues as you age is much higher.
Plans for health insurance coverage to mothers offer insurance for all pregnancy-related costs for the covered. These include costs associated with the normal or cesarean birth and postnatal or prenatal expenses and vaccinations for babies.
What is maternity insurance?
It is insurance that covers all costs associated with the birth of a child up to a specified time.
It is possible to choose a stand-alone policy or add it as an added health insurance plan with maternity insurance at a cost.
Maternity insurance provides maternity health coverage, covering costs associated with your child’s birth and the pregnancy. It’s not just about assisting with finances during pregnancy. But will also offer support following the birth, but it’s only for a specified time. With this program, mothers do not need to be concerned about their finances and can get the best medical care they can get.
What’s covered by the maternity insurance plan?
Maternity Insurance covers all expenses up to a specific predefined limit on your delivery. The insurance is available for both normal and Caesarean deliveries. Specific policies might cover the cost of termination due to complications. Certain insurance provides pre and post-natal and newborn baby coverage with the amount of maternity insurance.
Expenses During Delivery & Labor:
All expenses made, up to the amount of the insurance, are covered under the insurance for mothers.
Caesarean Delivery:
C-section and caesarean deliveries are a procedure used to birth the baby when a vaginal birth is unsafe for the mother or the baby. It is covered under pregnancy insurance.
Cover for Baby’s new arrival:
The maternity insurance will protect your newborn baby for the initial 90 days (check for the exact same information from your insurance provider) and handle vaccinations and any other complications.
Treatment for Infertility:
If both of you are having fertility issues, the insurance company will cover the cost of treatment for infertility.
Problem during pregnancy:
Some women experience medical problems and require treatment for them. Pregnancy-related complications are covered by your insurance.
Room Rent:
The hospitalisation and costs for the room will be covered by medical insurance.
Terminations:
In some cases, the termination of pregnancy could be recommended due to medical conditions. The costs you incur for legal terminations are paid for.
What is not covered in Pregnancy Health Insurance?
Certain services are not part of your maternity insurance. They are known as exclusions. Storage and harvesting of stem cells are performed to avoid possible diseases from occurring in the future. The expenses incurred due to ectopic pregnancy are not covered under pregnancy coverage. This could be covered by the individual health insurance plan. If the postnatal and prenatal checks require hospitalisation, your maternity insurance will not be able to cover the cost.
Is pregnancy considered a pre-existing condition for health insurance?
The majority of insurance companies don’t provide coverage for maternity even if you’re already expecting. They view the pregnancy as an existing condition beyond insurance coverage.
Are you able to get health insurance if you’re pregnant?
You can avail of health insurance if you’re expecting. If you’re contemplating when you should get pregnant coverage, it is recommended that you don’t delay the decision.
This is because pregnant insurance with no waiting time isn’t readily accessible. In general, you must wait for about three or four years to avail the benefits of this insurance.
How is the maternity insurance premium determined?
The cost of an insurance policy for maternity is more expensive than a standard Medical Insurance policy. The probability of a claim being made in the context of the insurance policy is 100, which is why insurance companies have a higher cost for the policies. If you are considering purchasing the insurance plan, it is advised to perform a cost-benefit study of the various options offered by multiple insurance companies. It is important to keep in mind that the price of pregnant insurance rises as you get older. Additionally, the costs associated with pregnancy are increasing each day. To make sure you can get a low-cost plan with the most advantages, it’s best to get one today and don’t put off making a choice.
Exclusions and inclusions included in Maternity Benefit plan:
Exclusions are situations where the policyholder can’t make any claim against maternity benefits. These are the exclusions for pregnant coverage:
Inclusions:
Tests, Costs for ambulance services, Medication, Inpatient treatment, Pre-natal costs, Follow-up visits, Daycare, Post-natal costs, Room rent, Caesarean/normal delivery, Cover for a newborn baby
Cost of treatment for infertility. Costs associated with tonics, vitamins, or other supplements. A pregnancy that isn’t included in the base plan. The Claim was raised at the time of waiting. The Claim is filed when the permitted number of claims exceeds.
Exclusions:
Tests and treatments for IVF, Self-inflicted injuries, Pre-existing diseases
Post-hospitalization and pre-hospitalization coverage:
Hospitalization expenses
Cost of a medically needed termination of pregnancy in a potentially life-threatening scenario. Cost of regular and cesarean delivery. Protection for newborn babies The baby’s birth is protected under maternity benefits until 90 days after birth, at no cost. Once the infant is 90 days old, it has to be covered under the basic policy as insurance. Protection for vaccinations The newborn baby has to be protected at intervals. The costs for standard and reasonable vaccines are covered by the maternity benefits offered by the health insurance plan.
The following vaccinations are covered by the plan:
BCG ,OPV+IPV-B1/OPV, Hepatitis B-1, DTPw booster-1 DTPa booster-1,Hib, Measles,MMR-1,Typhoid,HPV (female child),Meningococcal, Tetanus Toxoid.
Why should you purchase Maternity Health Insurance Coverage?
A maternity health insurance policy can provide peace of mind regarding cost-related expenses associated with your child. When purchased, the coverage is available with a minimal cost as an additional benefit to your health insurance plan and offers adequate financial protection for hospitalization and maternity expenses. Here are some of the reasons to consider taking advantage of maternity insurance.
Financial Coverage:
The expenses associated with birth and childbirth can be 50 to 1 lakh rupees in certain parts of India. The cost could be related to the standard of healthcare services provided during this period. It is possible to say that purchasing pregnancy insurance will provide better health care facilities for the pregnant mother and child. Therefore, the significance of having insurance is significant.
Surgery-related Deliveries are more expensive:
Cesarean or surgical delivery is when the normal childbirth process is deemed challenging for both the mother and the baby. This is when medical intervention is required for the infant to be delivered through a major abdominal procedure. The decision to have a cesarean birth can be done at any time. The price of the procedure is significantly more expensive than an ordinary delivery. These costs are covered under the Mediclaim policy, which includes maternity coverage.
Peace of Mind
After the financial burden is diminished by maternity insurance, the parents can concentrate on the important event in their own lives. Making plans for naming the baby decorating the nursery, hosting baby shower parties, and much more can be accomplished without worrying.
The best time to choose Pregnancy Insurance?
The best thing to do is buy health insurance and buy health as soon as possible. The earlier you purchase health insurance, the less expensive it will cost. Be aware that you’re the older person today but younger than the next day. It is now the time to buy health insurance. Maternity plans are an added-on that you can purchase when you are married, i.e. during the middle of your policy term or after your health insurance renewal.
Maternity coverage includes a waiting period. The time frame for waiting can differ from one insurer to the next. Certain insurance companies have a waiting period of nine months following the purchase of the maternity package, while other companies have a waiting time of several years. You must speak to your insurance company to inquire how long you have to wait for the period. Maternity insurance policies, also known as maternity insurance, are accessible through Group Health Insurance plans. For example, Employee health insurance schemes. They usually don’t include a waiting clause. An employee who is a permanent member of a company may file a claim for maternity benefits without waiting for a certain time.
Who should choose Maternity Benefit option?
If you’re newlyweds, this plan is an absolute must for you, as it is possible that you will decide to have a child in the future, and this plan will assist you in finance that moment. You should also be aware that typically there is a waiting time of 9 months to 3 years. You aren’t able to claim any benefits during this time. This is why it’s recommended to purchase this plan as soon as you can so that once you’re looking to begin your family, you do not have to be concerned about waiting time. There is also an age restriction to purchasing this plan. Anyone between 18 and 45 is eligible to purchase the plan. The policy covers these cases for group members.
Tax Benefits Associated with Maternity Coverage
The health insurance plan provides an income tax benefit of Rs 25000 for a single calendar year (the amount could change based on the regulations) in the case of the Indian taxpayer.
Because maternity insurance is an additional benefit in the insurance plan, it’s already covered by tax benefits. There aren’t any tax exemptions when purchasing pregnant health insurance plans.
How do I Claim Process to avail of Maternity Benefits?
The issue of the maternity benefit may be made in one of two methods: There are two methods you can claim:
Cashless Claim:
It is essential to have the delivery take place at a hospital that is a member of the network to be eligible for the benefit of a payment that is cashless. The term “network hospital” refers to a hospital with a tie-up in conjunction with your health insurance provider.
The insurance company must be informed of the claim before you are admitted to a network hospital. After the claim has been approved, the insured must pay a small amount of the deductible, and no further action is needed. The other costs will be handled in the direct hands of an insurance provider.
If you’re getting your treatment in one of the hospitals in the network. You can submit cashless claims. Simply bring your Health/Policy card to the Helpdesk and complete the cashless Claim request form.
Complete the form with other documents required, after which the hospital, along with TPA, Third-Party Association, will then take it from there. Your documents and forms will be inspected, and if everything is in order, your claim will shortly be handled.
Reimbursement Claim:
Reimbursement claims require the insured to first pay the full amount due and then contact the insurance company to request reimbursement of costs. This is a long process in comparison to cashless processes.
For this type of case, the insured is not limited to receiving treatment at a hospital part of the network. The treatment can take place at any hospital that the insured chooses. The insured must keep track of all documents and bills to file a reimbursement claim.
If the maternity benefits are purchased by a digital insurer, the policyholder can file a claim for medical expenses associated with maternity online, i.e. through a website or mobile application.
If you were unable to go to an affiliated hospital and went to a non-network facility, you must inform your insurance provider within the first 24 hours after your hospitalization. The hospital and TPA will review the documentation, and if all is in order, your claim will be reviewed, and the money you paid for your treatment will be returned to your account.
Documents required to apply for Maternity Insurance
The following documents are needed when making a claim:
- Policy Paper
- Health/Policy Card
- Form for pre-authorization
- KYC Document
- Claim Form
- Discharge Summary
- Medicine prescriptions
- Other Document as required by Insurance Company